Home Tags Posts tagged with "vaccination"
vaccination
When Donald Trump claimed, in the second Republican debate, that vaccines may be linked to autism, he stirred a dispute that began in 1998 and had long been debunked.
Such is the way of the Republican party. Dig up old and discredited arguments. Dust them off and present them as shiny and new.
The approach may not be as harmful when it comes to economic policy, but when it comes to something as potentially life-saving — and life-threatening — as vaccines, then Trump needs to get up-to-date.
The scene of Trump talking about vaccines and autism was unsettlingly familiar.
Many infectious disease specialists have spent their career trying to reveal the lie in the contention that shots can cause severe medical conditions.
A Money Grab?
Years ago, an American traveling overseas would be shown a diagram of where vaccinations were a must. The map designated every country in blue as being one that a visitor must have injections to travel safely. At the same time, Europeans going overseas were also shown a similar representation.
There were just two differences. On the American’s map, every country was shaded blue except the USA. The European tourist’s guide showed every nation in blue — except Europe.
A conspiracy theorist would enjoy explaining the international drive for inoculations — when people travel. You may not be a conspiracy theorist but don’t ignore the idea that all travel vaccinations are suggested with something other than health being the top priority.
Travel anywhere requires documentation that the visitor has had their travel vaccinations. Written evidence of immunization can even be drilled down to the level of what region in which a person traveled. For instance, if a person has just visited a nation with a yellow fever concern — which includes much of South America, they may be obligated to show evidence of vaccination before entering another later. It is seldom asked for, except for yellow fever, but sometimes needed.
Vaccine Or Not To Vaccine
Dr. Randall Neustaedter, the author of The Vaccine Guide, offers three simple prerequisites in deciding about travel vaccines: risk, potential vs. likelihood and efficiency.
Risk
Determine which illnesses you may be at risk for in the area you are traveling. Some nations require proof, but most only recommend and don’t require. The latest vaccine recommendations can be found on the official CDC website.
Potential vs. Likelihood
Think about the likelihood of catching an illness compared to possible side effects of a vaccine. While it doesn’t make sense to get an unneeded vaccine, determine if the risks outweigh the shot.
Efficiency
Consider the efficacy rate of the vaccine you’re studying. It’s simple. What can you catch? How likely are you to catch it and what are the side effects?
Neustaedter says Hepatitis A, typhoid, and yellow fever are the three usually considered for travel vaccinations.
Hepatitis A
A viral infection affecting the liver. Rarely fatal and doesn’t cause chronic illness. Commonly acquired by consuming contaminated water, rice or raw foods.
Typhoid
Contracted through water contaminated by sewage. Typhoid is most often acquired in underdeveloped tropical areas of Latin America and Africa.
Yellow Fever
A severe viral disease transmitted between humans via mosquitoes. The sickness is fatal if not treated. Over 100 nations require proof of vaccination for yellow fever below entering — even layovers which last more than twelve hours.
Considerations For Vaccinations Prior To Overseas Travel
Pregnancy
Tetanus, diphtheria and pertussis vaccines should be given during pregnancy irredgardless of the woman’s travel plans. The CDC recommends vaccinations if f a travel itinerary is fixed and specific regions cannot be avoided. The risks for exposure are often believed to outweigh the risks of vaccination.
Children
Vaccinating children for travel requires serious consideration. When possible, children should complete the routine immunizations of childhood on a regular schedule. Travel at a younger age may demand an accelerated timetable of shots and the CDC says not all travel-related shots are useful in infants. In fact, some are specifically contraindicated.
Elderly
Vaccines.gov suggests those over 65 often need one or more vaccines, including:
Influenza (Flu)
Shingles (Herpes Zoster)
Diphtheria
Tetanus
Pertussis (Whooping Cough)
Pneumococcal disease (Pneumonia)
Compromised Immune System
The CDC Travelers Health site lists what vaccines are recommended based on the destination for those with autoimmune disorders. While most vaccines are made from killed bacteria viruses and are safe, they may be less efficient in persons with abnormal immune systems, leaving them unprotected or not adequately protected.
More than 350 Chinese officials are to face punishment over a scandal involving the illegal sale of vaccines.
According to the Xinhua news agency, 192 criminal cases had been filed over the case, which saw improperly stored or transported vaccines sent to 59 health institutions.
The government has said it will tighten procedures around vaccine-handling.
The vaccine scandal has caused widespread anger in China.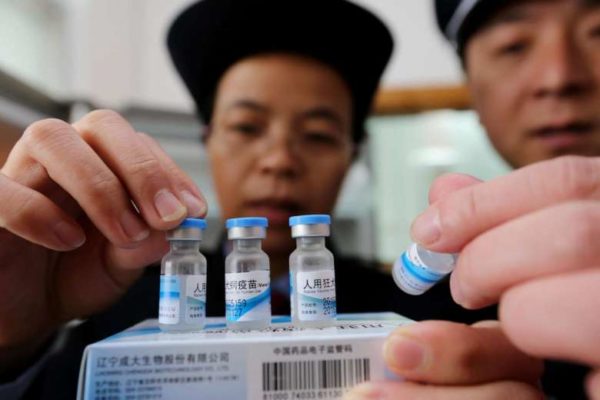
The illegal vaccine ring was reportedly in operation since 2011, and in April 2015 two women were arrested for selling some $88 million worth of vaccines.
However, the details were only made public last month, when the authorities issued a call demanding that suppliers come forward to help them trace potential victims.
China’s State Council said the 357 officials faced demotion or losing their jobs and that 202 had been detained so far.
Health authorities have also urged people to continue coming forward for vaccinations.
The China office of t
The World Health Organization (WHO) in China has said vaccines needed to be handled properly or they can become less effective.
It stressed that improperly kept vaccines did not in themselves present much danger.
A universal flu vaccine comes closer after promising trials in animals, scientists have announced.
According to researchers, the vaccine would give life-long protection against any type of flu.
Two separate teams have found success with an approach that homes in on a stable part of the flu virus.
That should remove the problem with current flu vaccines which must be given anew each year because they focus on the mutating part of the virus.
The proof-of-concept work is published in Science journal and Nature Medicine.
The US studies are now needed in humans to confirm that the method will work in man.
In the meantime, experts say people should continue to receive an annual flu jab because vaccination is still the best way to protect yourself against infection.
Conventional flu jabs target molecules on the surface of the flu virus, but these are constantly changing.
It is the stems that scientists are now focusing on as a target for a universal flu jab.
India has announced polio eradication after three years since its last reported case, a landmark in the global battle against the disease.
It is seen as confirmation of one of India’s biggest public health successes, achieved through a massive and sustained immunization program.
India’s health minister hailed it as a “monumental milestone”.
In 2012 the World Health Organization (WHO) removed India from the list of polio-endemic countries. Pakistan, Afghanistan and Nigeria remain on it.
The list refers to countries in which the virus is circulating freely and the transmission of the infectious disease has not been stopped.
Despite India’s success, health experts fear a resurgence of polio in other parts of the world.
“This monumental milestone was possible due to unwavering political will at the highest level, commitment of adequate financial resources, technological innovation … and the tireless efforts of millions of workers including more than 23 lakh (2.3 million) vaccinators,” Health Minister Ghulam Nabi Azad told reporters.

India is marking three years since its last reported polio case
The WHO is expected to formally certify India’s polio-free status next month after testing its last samples.
“India has now set other important public health goals as a result of the confidence that the country has got from the successful eradication of polio,” the WHO’s Hamid Jafari told AFP news agency, citing a new goal to eradicate measles.
Only one case of polio was recorded in India in 2011, down from 741 in 2009. It came from the eastern state of West Bengal in 2011 when an 18-month-old girl was found to have contracted the disease.
After the eradication of smallpox in 1980, polio is the second disease in India that has been eliminated through immunization.
Nearly 2.3 million volunteers vaccinate some 170 million children under five years of age in India during every round of immunization.
Polio is capable of causing crippling disability or death within hours. It plagued societies in ancient times – and was present in more than 100 countries even in the 1980s, when it left 350,000 people paralyzed each year.
Global cases have decreased since then as part of a mass eradication program – to 372 in 2013.
[youtube C7WKBLtAO_c 650]
Katie Couric has admitted a disproportionate reporting on HPV vaccine controversy during an episode of her show.
She said some of the criticism that the episode was too anti-vaccine and anti-science “was valid”.
“We simply spent too much time on the serious adverse events that have been reported in very rare cases following the vaccine,” Katie Couric wrote in a blog post published Huffington Post.
“More emphasis should have been given to the safety and efficacy of the HPV vaccines.”
The December 4 episode of Katie show had been criticized for promoting arguments from moms who said their daughters were harmed by the vaccines, including one whose child died. Katie Couric also interviewed HPV researcher Dr. Diane Harper, chair of family medicine at the University of Louisville. Harper had researched the vaccine and said its protection would wear off after five years.
Experts were quick to point out that scientific evidence didn’t jive with the opinions from Katie Couric’s guests.

Katie Couric has admitted a disproportionate reporting on HPV vaccine controversy
For the 57 million doses of the vaccine given out from June 2006 through March 2013, the Centers for Disease Control and Prevention’s Vaccine Adverse Event Reporting System (VAERS) has received at least 22,000 reports of adverse events in girls and women. About 92 percent of which were classified as non-serious. The other almost 8% of serious side effects included headache, nausea, vomiting, fatigue, dizziness, fainting and generalized weakness.
Katie Couric’s blog post devoted more space to the science. She highlighted the risk between HPV and cancer, citing estimates that each year about 26,000 Americans are diagnosed with a cancer caused by HPV.
She noted that while the vast majority of side effects to the HPV vaccine are not serious, she said she still felt the need to share the two patient stories on her show.
“As a journalist, I felt that we couldn’t simply ignore these reports. That’s why we had two mothers on the show who reported adverse reactions after their daughters had been vaccinated for HPV,” she wrote.
“One could hardly get out of bed for three years, and the other tragically died. There is no definitive proof that these two situations were related to the vaccine. Every life is important. However, the time spent telling these stories was disproportionate to the statistical risk attendant to the vaccines and greater perspective is needed.”
She added that as a cancer-prevention advocate, one of her goals was to affirm the importance of getting Pap tests and that people should not skip gynecological visits just because they got an HPV vaccine.
Katie Couric also expressed support for the vaccine, adding her own two daughters had been vaccinated.
The WHO has confirmed 10 cases of polio in Syria – the first outbreak in the country in 14 years.
The WHO says a further 12 cases are still being investigated. Most of the 22 people who have been tested are babies and toddlers.
Before Syria’s civil war began in 2011, some 95% of children were vaccinated against the disease.
The UN now estimates 500,000 children have not been immunized.
The WHO said the suspected outbreak centres on the eastern province of Deir Ezzor.
The highly contagious disease is most often spread by consuming food or liquid contaminated with faeces.
“Of course this is a communicable disease, with population movements it can travel to other areas. So the risk is high for [its] spread across the region,” the Reuters news agency quotes WHO spokesman Oliver Rosenbauer as saying in Geneva.
“Immunizations have started in that area,” he said.
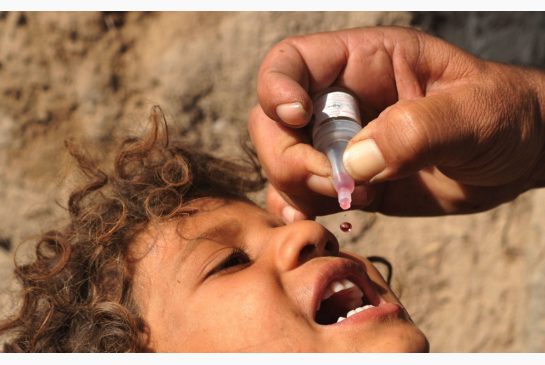
The WHO has confirmed 10 cases of polio in Syria
There are more than 100,000 children, all under age five, now at risk of polio in Deir Ezzor province alone, which has been caught in fierce battles between Syrian government forces and opposition fighters.
The city of Deir Ezzor remains partially controlled by forces loyal to President Bashar al-Assad, while the countryside is in the hands of the opposition.
More than 4 million Syrians have been displaced internally by the conflict and generally live in overcrowded, unsanitary conditions.
A further two million have fled the country, many of them living in refugee camps in Jordan, Lebanon, Turkey and Egypt.
The WHO has already reported increases in cases of measles, typhoid and hepatitis A.
Since the first suspected polio case was reported 10 days ago, Syria’s Health Ministry has begun an immunization drive and aid agencies have begun developing emergency immunization plans at Syrian refugee camps.
Oliver Rosenbauer said most victims were under two years old and were thought never to have been vaccinated against polio.
“The next step will be to look genetically at these isolated viruses and where they came from. That should give some clarity on the origin,” he said.
Polio has been largely eradicated in developed countries but remains endemic in Nigeria, Pakistan and Afghanistan.
There is no known cure, though a series of vaccinations can confer immunity.
Young children are particularly susceptible to paralytic polio, the most serious form of the disease.
What is polio?
- Polio (poliomyelitis) mainly affects children aged under five
- It is a highly infectious disease caused by a virus which invades the nervous system
- Symptoms include fever, fatigue, headache, vomiting, stiffness in the neck, and limb pain
- One in 200 infections leads to irreversible paralysis
- Between 5-10% of those who suffer paralysis die because their breathing muscles are immobilized
- Cases have fallen by over 99% since 1988, from around 350,000 then to 223 in 2012
- However polio remains endemic in Afghanistan, Nigeria and Pakistan
Source: World Health Organization
[youtube fa15uarEuPw 650]
The most ambitious goal of medical researchers is to find ways to prevent diseases. Methods to accomplish that goal do exist for certain illnesses, but are rare for others. Two recent medical studies on the molecular level exemplify the effort of the scientists to contribute to strengthening it against organ failure and to immunizing the body against viruses.
Avoiding a bad heart condition
In the US, 1.5 million people suffer from a heart attack each year of which one third is killed by it. Scientists of the Lund University in Sweden have now discovered a way to reduce the risk of a heart attack through a vaccination. The researchers have developed a therapy which leads to the production of antibodies attacking the accumulation of fat deposits in the arteries. Such therapies are often the result of comprehensive research collaborations on an international level, and also rely on the recommendation by the antibody supplier, which provides the appropriate kits for long-term clinical studies. The promising research results are hoped to lead to an introduction of the antibody therapy within the next five years.
A vaccine against cervical cancer
The vaccination Cervarix was approved in various European countries and the US between 2007 and 2009. It has been a great success as it immunizes the body against certain types of the Human Papillomavirus which were proved to be the cause of genital warts and cervical cancer by the German researcher Harald zur Hausen. Since its approval, many young girls and boys have got the three necessary injections and have thereby reduced their risk to fall ill to cervical, vaginal, penile, vulvae and anal cancer.
New results in the prevention of cervical cancer
In order to optimize the vaccine, scientists continue studying its effects in relation to the virus. It has been found out recently that even people who do not get the shot may profit from it through the phenomenon of herd immunity. It is related to the fact that vaccinated people do not transmit the virus to their potentially unvaccinated sexual partners and thereby help reduce the circulation of the virus. Hence, the virus may disappear or get extinct over time. This fact, however, should not prevent young people from getting vaccinated themselves. After all, one does not always know if a sexual partner is immunized or not.
On top of that, it has to be noted that there are still some oncogenic types of the Human Papillomavirus which are not covered by the current vaccines. It therefore remains the challenge of the scientists to develop serums to cover a broader range of HPV virus.
US researchers say smokers could one day be immunized against nicotine so they gain no pleasure from the habit.
They have devised a vaccine that floods the body with an antibody to assault nicotine entering the body.
A study in mice, published in Science Translational Medicine, showed levels of the chemical in the brain were reduced by 85% after vaccination.
Years of research are still needed before it could be tested on people.
However, lead researcher Prof. Ronald Crystal is convinced there will be benefits.
“As far as we can see, the best way to treat chronic nicotine addiction from smoking is to have these Pacman-like antibodies on patrol, clearing the blood as needed before nicotine can have any biological effect.”

US researchers say smokers could one day be immunized against nicotine so they gain no pleasure from the habit
Other “smoking vaccines” have been developed that train the immune system to produce antibodies that bind to nicotine – it is the same method used to vaccinate against diseases. The challenge has been to produce enough antibodies to stop the drug entering the brain and delivering its pleasurable hit.
Scientists at Weill Cornell Medical College have used a completely different approach, a gene-therapy vaccine, which they say is more promising.
A genetically modified virus containing the instructions for making nicotine antibodies is used to infect the liver. This turns the organ into a factory producing the antibodies.
The research team compared the amount of nicotine in the brains of normal mice with those that had been immunized. After being injected with nicotine, the vaccinated mice had nicotine levels 85% lower.
It is not known if this could be repeated in humans or if this level of reduction would be enough to help people quit.
Prof. Ronald Crystal said that if such a vaccine could be developed then people “will know if they start smoking again, they will receive no pleasure from it due to the nicotine vaccine, and that can help them kick the habit”.
He added: “We are very hopeful that this kind of vaccine strategy can finally help the millions of smokers who have tried to stop, exhausting all the methods on the market today, but find their nicotine addiction to be strong enough to overcome these current approaches.”
There are also issues around the safety of gene therapy in humans that will need to be answered.
If such a vaccine was developed it could also raise ethical questions about vaccinating people, possibly in childhood, before they even started smoking.
A vaccine against one of the most common forms of childhood meningitis could reduce the number of deaths in the world.
The current vaccination programme protects against only some of the bacterial types involved.
A Chilean study, reported in The Lancet medical journal, found more evidence the new vaccine works against the B form of the disease.
This causes about 2,000 cases in the UK each year, mostly in the under-fives.
The meningitis vaccine programme here is thought to have saved many hundreds of lives over the past decade.
However, meningitis B has been an elusive target for vaccine developers, as it is a group of thousands of subtly-different strains of bacteria, making it difficult to find a single jab that could cover them all.
So while four other major strains are included in the vaccine, the danger from meningitis B remains.
The infection, which causes inflammation of membranes surrounding the spinal cord and brain, still causes more than 100 deaths a year, with many more children suffering serious and potentially disabling illness.

Meningitis B has been an elusive target for vaccine developers, as it is a group of thousands of subtly-different strains of bacteria, making it difficult to find a single jab that could cover them all
Scientists produced the “4CMenB” vaccine by analyzing the genetic structure of thousands of B strains, looking for shared features which could be targeted.
There have already been encouraging results when given to toddlers, and the latest study, carried out by University of Chile scientists, looked at its effectiveness when given to 11 to 17-year-olds.
More than 60% of bacterial meningitis cases in Chile involve type B, but two doses of the vaccine appeared to offer almost 100% protection.
The researchers said that the vaccine could now be considered for vaccination programmes in countries where the B type was prevalent, including many in Europe, and the United States.
Dr. Myron Christodoulides, a senior lecturer in Molecular Microbiology at the University of Southampton, said that the full range of type B strains covered by the vaccine was not yet proven.
He said: “Previous studies have shown that 4CMenB has the potential to provide significant protection when administered to infants – this new study shows it could also be highly protective in the adolescent age group.
“However, there are still a number of important questions to be answered such as how many strains it will protect against, how long the protection will last and whether it will stop the bacteria from being passed on to others, providing indirect protection to those not vaccinated.”








