According to Canadian scientists, being exposed to “good bacteria” early in life could prevent asthma developing.
The research team, reporting in Science Translational Medicine, were analyzing the billions of bugs that naturally call the human body home.
Their analysis of 319 children showed they were at higher risk of asthma if four types of bacteria were missing.
Experts said the “right bugs at the right time” could be the best way of preventing allergies and asthma.
In the body, bacteria, fungi and viruses outnumber human cells 10 to one, and this “microbiome” is thought to have a huge impact on health.
The specialists, at the University of British Columbia and the Children’s Hospital in Vancouver, compared the microbiome at three months and at one year with asthma risk at the age of three.
Children lacking four types of bacteria – Faecalibacterium, Lachnospira, Veillonella, and Rothia (Flvr) – at three months were at high risk of developing asthma at the age of three, based on wheeze and skin allergy tests.
The same effect was not noticed in the microbiome of one-year-olds, suggesting that the first few months of life are crucial.
Further experiments showed that giving the bacterial cocktail to previously germ-free mice reduced inflammation in the airways of their pups.
One of the researchers, Dr. Stuart Turvey, said: “Our longer-term vision would be that children in early life could be supplemented with Flvr to look to prevent the ultimate development of asthma
“I want to emphasize that we are not ready for that yet, we know very little about these bacteria, [but] our ultimate vision of the future would be to prevent this disease.”
Asthma is caused by airways that are more sensitive to irritation and inflammation.
One explanation for the rise in asthma and allergies is the “hygiene hypothesis”, which suggests that children are no longer exposed to enough microbes to calibrate the immune system to tell the difference between friend and foe.
Giving birth by Caesarean section and not breast-feeding both limit the bacteria that are passed to a newborn. Antibiotics taken by a pregnant woman or newborn child can also change the microbiome.
Dr. Brett Finlay, another researcher in the project, said: “[I was] surprised to realize that fecal microbes may be influencing things.
“What data’s really starting to show these days is that the immune system gets itself set up in the gut and influences how it works everywhere else in the body.”
[googlead tip=”patrat_mediu” aliniat=”stanga”]A new treatment for leukemia had amazing results, surprising even the researchers who designed it. The new treatment has eradicated the cancer cells present in the first three patients tested bodies.
Early results of a clinical trial showed that genetically engineered T cells eradicate leukemia cells and thrive.
Scientists from the University of Pennsylvania have genetically engineered patients’ T cells — a type of white blood cell — to attack cancer cells in advanced cases of a common type of leukemia.
The first two of three patients studied, who received the innovative treatment, have been cancer-free for more than one year. In the case of the third patient, over 70% of cancer cells were removed, according to the researchers.
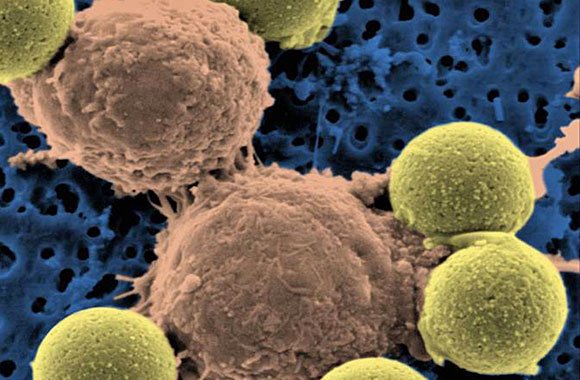
"Microscopic image showing two T cells binding to beads, depicted in yellow, that cause the cells to divide. After the beads are removed, the T cells are infused into cancer patients." (Dr. Carl June / Pennsylvania Medicine)
“In just three weeks, tumors were destroyed, the effect being more violent than we ever have imagined,” said Dr. Carl June, one of the researchers involved in the study.
“Each cell can destroyed thousands of cancer cells,” said June, “each patient have been removed tumors from at least 900 grams.”
“A huge accomplishment”
[googlead tip=”vertical_mare” aliniat=”dreapta”] “This is a huge accomplishment — huge,” said Dr. Lee M. Nadler, dean for clinical and translational research at Harvard Medical School, who discovered the molecule on cancer cells that the Pennsylvania team’s engineered T cells target.
Innovative treatment is using patients’ own T cells, which are extracted from body cells and then genetically modified to attack cancer cells and to multiply and then reintroduced into patients’ blood.
Findings of the trial were reported Wednesday in the New England Journal of Medicine and Science Translational Medicine.
According to LA Times report, for building the cancer-attacking cells, the researchers modified a virus to carry instructions for making a molecule that binds with leukemia cells and directs T cells to kill them. Then they drew blood from three patients who suffered from chronic lymphocytic leukemia and infected their T cells with the virus.
When they infused the blood back into the patients, the engineered T cells successfully eradicated cancer cells, multiplied to more than 1,000 times in number and survived for months. They even produced dormant “memory” T cells that might spring back to life if the cancer was to return.
On average, the team calculated, each engineered T cell eradicated at least 1,000 cancer cells.
Side effects included loss of normal B cells, another type of white blood cell, which are also attacked by the modified T cells, and tumor lysis syndrome, a complication caused by the breakdown of cancer cells.
“We knew [the therapy] could be very potent,” said Dr. David Porter, director of the blood and marrow transplantation program at the Hospital of the University of Pennsylvania in Philadelphia and a coauthor of both papers, which were published in the New England Journal of Medicine and Science Translational Medicine.
“But I don’t think we expected it to be this dramatic on this go-around.”
Bone marrow transplants from healthy donors have been effective in fighting some cancers, including chronic lymphocytic leukemia, but the treatment can cause side effects such as infections, liver and lung damage, even death.
“1/5 of bone marrow transplant recipients may die of complications unrelated to their cancer,” Porter said.
Researchers have been working for many years to develop cancer treatments that leverage a patient’s immune system to kill tumors with much greater precision.
Specialists not involved in the trial said the new discovery is very important because it suggested that T cells could be adapted to destroy a range of cancer cells, including ones of the blood, breast or colon
“It is kind of a holy grail,” said Dr. Gary Schiller, a researcher from UCLA’s Jonsson Comprehensive Cancer Center who was not involved in the trial.
“It would be great if this could be applied to acute leukemia, where there is a terrible unmet medical need,” UCLA’s Schiller said.
Dr. David Porter added:
“Previously efforts to replace risky bone marrow transplants with such engineered T cells proved disappointing because the cells were unable to multiply or survive in patients.”
“This time, the T cells were more robust because the team added extra instructions to their virus to help the T cells multiply, survive and attack more aggressively.”
“About 15,000 patients are diagnosed with chronic lymphocytic leukemia every year. Many can live with the disease for years. Bone marrow transplants are the only treatment that eradicates the cancer.”
[googlead tip=”lista_mare” aliniat=”stanga”]Dr. David Porter cautioned that these were preliminary results and the scientists plan to continue the trial, treating more patients and following them over longer periods.
“The researchers also would like to expand the work to other tumor types and diseases,” Porter said.
The hope, scientists said, is that the method would work for cancers that can kill more ruthlessly and rapidly.


