Home Tags Posts tagged with "New England Journal of Medicine"
New England Journal of Medicine
A British study suggests that an early exposure to peanut products dramatically cuts the risk of allergy.
Doctors found that exposing at risk infants to peanuts before their first birthday lower the risk of developing a peanut allergy.
Trials on 628 babies prone to developing peanut allergy found the risk was cut by over 80%.
The King’s College London researchers said it was the “first time” that allergy development had been reduced.
Specialists said the findings could apply to other allergies and may change diets around, but warned parents not to experiment at home.
The research team in London had previously found that Jewish children in Israel who started eating peanuts earlier in life had allergy levels 10 times lower than Jewish children in the UK.
The trial, reported in the New England Journal of Medicine, focused on babies as young as four months who had already developed eczema – an early warning sign of allergies.
Skin-prick tests were used to identify those who had not yet developed peanut allergy or had only a very mild response.
Children under five should not eat whole peanuts, because of the risk of choking, so half were given a peanut-based snack. The other half continued avoiding peanuts.
The trial indicated that for every 100 children, 14 would normally go on to develop an allergy by the age of five.
This fell by 86% to just two out of every 100 children with the therapy.
Even the children who were already becoming sensitive to peanuts benefited. Their allergy rates fell from 35% to 11%.
Until 2008, at-risk families were told to actively avoid peanut products and other sources of allergic reactions.
The study findings have attracted excited responses from other doctors, and there is speculation similar approaches might work with other allergies, such as egg protein.
[youtube gLhHL8pjYRc 650]
US researchers claim that omelettes, meringues and pasta could one-day be back on the menu for some people with egg allergies after they are treated with the food they are allergic to.
The only option for patients is to completely avoid foods containing egg.
A study on 55 children showed some were able to eat egg after minuscule amounts were gradually added to their diets.
However, the treatment is still experimental and doctors say it should not be tried at home.
Egg allergies are one of the most common allergies and are thought to affect up to 2.5% of children.

Egg allergies are one of the most common allergies and are thought to affect up to 2.5 percent of children
Gradually introducing the food which causes an allergic reaction has been successful in other foods such as such as peanuts.
Parents were given powdered egg to mix into their children’s food, building up to about a third of an egg every day.
The findings, presented in the New England Journal of Medicine, report that after 22 months of egg therapy, 75% of the children were able to eat the equivalent of two eggs without reacting.
The children were tested again after at least a month of no longer having the daily egg treatment. Of these, 28% could still eat egg without reacting and were considered allergy-free.
One of the researchers Dr. Wesley Burks, from the University of North Carolina School of Medicine, said: “This study gives us hope that we’re closer to developing a treatment.
“Almost a third of the children had a permanent change and were no longer egg-allergic.”
Dr. Stacie Jones, from University of Arkansas, said: “Reducing these kids’ allergic response to egg also lessened parental anxiety over how their children might react if accidentally exposed to egg at school or at someone else’s house.”
However, about 15% of children did not finish the treatment, mostly due to allergic reactions.
A team at Washington University School of Medicine has assembled a “timeline” of the unseen progress of Alzheimer’s before symptoms appear.
Scientists looked at families with a genetic risk of the disease.
Writing in the New England Journal of Medicine, they say signs appeared up to 25 years before the expected onset of the disease.
The 128 people in the study, from the UK, US and Australia, had a 50% chance of inheriting one of three mutations that are certain to cause early Alzheimer’s, which often develops in people’s 30s and 40s – much earlier than the more common form of Alzheimer’s which generally affects people in their 60s.
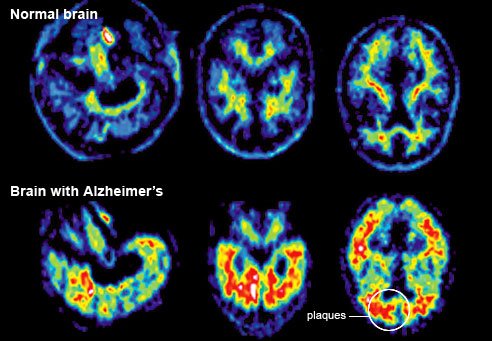
A team at Washington University School of Medicine has assembled a "timeline" of the unseen progress of Alzheimer's before symptoms appear
Those who carry the mutations will go on to develop the disease.
The researchers looked at the age the participants’ parents were when they developed the disease – and therefore how many years it was likely to be before they too showed symptoms.
They underwent blood and spinal fluid tests as well as brain scans and mental ability assessments.
The earliest change – a drop in spinal fluid levels of the key ingredient of Alzheimer’s brain plaques – can be detected 25 years before the anticipated age of disease onset, they suggest.
At 15 years, raised levels of tau, a structural protein in brain cells can be seen in spinal fluid – and shrinkage can also be detected within parts of the brain.
Changes in the brain’s use of the sugar glucose and slight memory problems become apparent 10 years before symptoms would appear, they suggest.
Researchers also tested other members of the families without the inherited mutations – and found no changes in the markers they tested for.
A new Australian study has found that fertility treatment used to help infertile men become fathers can raise the risk of birth defects in babies.
Research on more than 300,000 babies found those born using Intracytoplasmic sperm injection (ICSI) had a significantly higher risk of developing abnormalities than those conceived naturally.
Researchers linked a census of more than 6,100 births that occurred as a result of fertility treatment in South Australia to a registry of more than 300,000 births and 18,000 birth defects.
The report by the University of Adelaide published in the New England Journal of Medicine shows that on average defects were present in 8.3% of pregnancies that involved fertility treatment compared to 5.8% of those conceived naturally.
According to the study, in vitro fertilisation (IVF) posed the least risk to women opting for assisted conception, with defects occurring in only 7.2% of pregnancies.
ICSI is primarily used for male fertility problems and this risk is decreased using frozen eggs, according to the study’s lead author, Associate Professor Michael Davies.
“I don’t want to scare people,” he said because the majority of babies were born healthy.
“But this may be due to developmentally compromised embryos failing to survive the freeze/thaw process,” he said.
“While assisted reproductive technologies are associated with an increased risk of major birth defects overall, we found significant differences in risk between available treatments.”
Research on more than 300,000 babies found those born using Intracytoplasmic sperm injection (ICSI) had a significantly higher risk of developing abnormalities than those conceived naturally
More than 3.7 million babies are born each year through assisted reproduction.
Methods include everything from drugs to coax the ovaries to make eggs to artificial insemination and IVF. Fertility treatments account for about 4% of births in Australia and as many as 8% of them in Denmark, where costs are widely covered, Michael Davies said.
In the United States, more than 60,000 babies were born in 2009 from 146,000 IVF attempts. About three-quarters of them used ICSI, or intracytoplasmic sperm injection.
ICSI was developed because of male infertility. But half the time, it was not done for that reason but to improve the odds that at least some embryos will be created from an IVF attempt.
In 2005, the last year for which data was available, 5,935 babies were born as a result of IVF treatment compared to 5,265 babies born with the help of ICSI.
One surprising find within the research was a tripling of risk among women who used the drug clomiphene citrate to stimulate ovary production, though this was among a small group within the study.
The drug is cheap and easily available through the internet, raising the possibility of abuse, but it is known to cause foetal abnormalities if the woman taking is not aware she is already pregnant.
The drug is prescribed after a mandatory pregnancy test in a clinical setting, but this can be avoided in self-medication.
Associate Professor Michael Davies said: “While confined to a small group in our study, this is of particular concern as clomiphene citrate is now very widely available at low cost, and may easily be used contrary to manufacturers’ very specific instructions to avoid use if pregnant, as it may cause fetal malformations.
“This aspect of the study will need additional confirmation from future research.
“A history of infertility, either with or without assisted conception, was also significantly associated with birth defects.
“While factors associated with the causes of infertility explained the excess risk associated with IVF, the increased risk for a number of other treatments could not readily be explained by patient factors.
“ICSI, for instance, had a 57% increase in the odds of major defect, although the absolute size of the risk remained relatively small.”
A new study published in the New England Journal of Medicine found that patients who stayed on the dementia drug Aricept had a slower decline in their memory.
The new research suggests that thousands of patients with advanced Alzheimer’s disease could benefit from drugs.
Aricept (donepezil) tends not to be prescribed once sufferers progress beyond moderate symptoms.
The National Institute for Health and Clinical Excellence (NICE), the drugs regulator in UK, said its guidelines supported continuing treatment where there were benefits.
The patent for the medicine Aricept, which is used to treat Alzheimer’s disease, expired recently. Much cheaper versions under the generic name donepezil are already available for about £12 ($19) a month.
The researchers say their new evidence could lead to twice as many Alzheimer’s sufferers worldwide being given medication.
The trial involved 295 Alzheimer’s patients in England and Scotland who had been taking Aricept.
One set were given placebo tablets while another set stayed on Aricept. A third set were given another drug, Ebixa (memantine), which is usually prescribed only in the later stages of Alzheimer’s.
The fourth batch of patients received a combination of both drugs.
The researchers assessed each group for a year, looking at their cognitive scores on factors like memory, and also at how well they coped with everyday tasks such as dressing and eating.
A new study published in the New England Journal of Medicine found that patients who stayed on the dementia drug Aricept had a slower decline in their memory
Both drugs were unable to halt the decline of patients, but they slowed it down.
The study’s lead author, Professor Robert Howard from King’s College London Institute of Psychiatry, said: “For the first time, we have robust and compelling evidence that treatment with these drugs can continue to help patients at the more severe stages.
“Patients who continued taking donepezil were about four months ahead in how they were able to remember, communicate and perform daily tasks than those who stopped taking the drugs.
“It means a lot to doctors and carers to see differences like that. These improvements were sustained throughout the year.
“It’s fair to say that both drugs have independent, positive effects at this stage of dementia. I’m advising hospital colleagues to continue patients on donepezil, when it’s tolerated, and to add in memantine.”
About 500,000 people in the UK are thought to have Alzheimer’s disease – with only about 10% who are in the earlier stages currently on drug treatment.
[googlead tip=”patrat_mediu” aliniat=”stanga”]A new treatment for leukemia had amazing results, surprising even the researchers who designed it. The new treatment has eradicated the cancer cells present in the first three patients tested bodies.
Early results of a clinical trial showed that genetically engineered T cells eradicate leukemia cells and thrive.
Scientists from the University of Pennsylvania have genetically engineered patients’ T cells — a type of white blood cell — to attack cancer cells in advanced cases of a common type of leukemia.
The first two of three patients studied, who received the innovative treatment, have been cancer-free for more than one year. In the case of the third patient, over 70% of cancer cells were removed, according to the researchers.
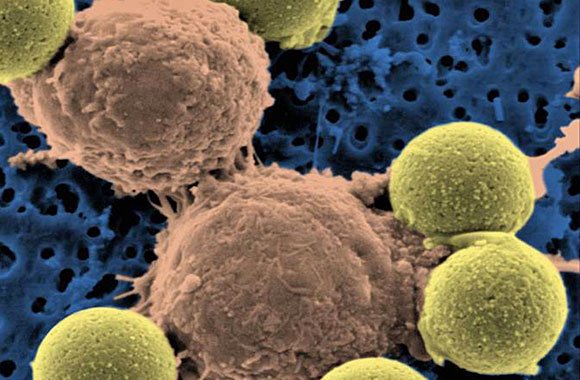
"Microscopic image showing two T cells binding to beads, depicted in yellow, that cause the cells to divide. After the beads are removed, the T cells are infused into cancer patients." (Dr. Carl June / Pennsylvania Medicine)
“In just three weeks, tumors were destroyed, the effect being more violent than we ever have imagined,” said Dr. Carl June, one of the researchers involved in the study.
“Each cell can destroyed thousands of cancer cells,” said June, “each patient have been removed tumors from at least 900 grams.”
“A huge accomplishment”
[googlead tip=”vertical_mare” aliniat=”dreapta”] “This is a huge accomplishment — huge,” said Dr. Lee M. Nadler, dean for clinical and translational research at Harvard Medical School, who discovered the molecule on cancer cells that the Pennsylvania team’s engineered T cells target.
Innovative treatment is using patients’ own T cells, which are extracted from body cells and then genetically modified to attack cancer cells and to multiply and then reintroduced into patients’ blood.
Findings of the trial were reported Wednesday in the New England Journal of Medicine and Science Translational Medicine.
According to LA Times report, for building the cancer-attacking cells, the researchers modified a virus to carry instructions for making a molecule that binds with leukemia cells and directs T cells to kill them. Then they drew blood from three patients who suffered from chronic lymphocytic leukemia and infected their T cells with the virus.
When they infused the blood back into the patients, the engineered T cells successfully eradicated cancer cells, multiplied to more than 1,000 times in number and survived for months. They even produced dormant “memory” T cells that might spring back to life if the cancer was to return.
On average, the team calculated, each engineered T cell eradicated at least 1,000 cancer cells.
Side effects included loss of normal B cells, another type of white blood cell, which are also attacked by the modified T cells, and tumor lysis syndrome, a complication caused by the breakdown of cancer cells.
“We knew [the therapy] could be very potent,” said Dr. David Porter, director of the blood and marrow transplantation program at the Hospital of the University of Pennsylvania in Philadelphia and a coauthor of both papers, which were published in the New England Journal of Medicine and Science Translational Medicine.
“But I don’t think we expected it to be this dramatic on this go-around.”
Bone marrow transplants from healthy donors have been effective in fighting some cancers, including chronic lymphocytic leukemia, but the treatment can cause side effects such as infections, liver and lung damage, even death.
“1/5 of bone marrow transplant recipients may die of complications unrelated to their cancer,” Porter said.
Researchers have been working for many years to develop cancer treatments that leverage a patient’s immune system to kill tumors with much greater precision.
Specialists not involved in the trial said the new discovery is very important because it suggested that T cells could be adapted to destroy a range of cancer cells, including ones of the blood, breast or colon
“It is kind of a holy grail,” said Dr. Gary Schiller, a researcher from UCLA’s Jonsson Comprehensive Cancer Center who was not involved in the trial.
“It would be great if this could be applied to acute leukemia, where there is a terrible unmet medical need,” UCLA’s Schiller said.
Dr. David Porter added:
“Previously efforts to replace risky bone marrow transplants with such engineered T cells proved disappointing because the cells were unable to multiply or survive in patients.”
“This time, the T cells were more robust because the team added extra instructions to their virus to help the T cells multiply, survive and attack more aggressively.”
“About 15,000 patients are diagnosed with chronic lymphocytic leukemia every year. Many can live with the disease for years. Bone marrow transplants are the only treatment that eradicates the cancer.”
[googlead tip=”lista_mare” aliniat=”stanga”]Dr. David Porter cautioned that these were preliminary results and the scientists plan to continue the trial, treating more patients and following them over longer periods.
“The researchers also would like to expand the work to other tumor types and diseases,” Porter said.
The hope, scientists said, is that the method would work for cancers that can kill more ruthlessly and rapidly.






