Combined therapy can help rare brain tumor patients to live more than a decade
Chemotherapy added to radiation therapy almost doubled the median survival time in patients with a rare form of brain tumor (oligodendroglioma) that carries a chromosomal abnormality (the 1p19q co-deletion), a study presented at the annual meeting of the Radiation Therapy Oncology Group showed.
The clinical trial was led by the Radiation Therapy Oncology Group (RTOG) with the participation of the North Central Cancer Treatment Group, the National Cancer Institute of Canada Clinical Trials Group, the Eastern Cooperative Oncology Group, and SWOG (formerly the Southwest Oncology Group).
The study enrolled 286 patients with aggressive brain tumors, oligodendrogliomas, who were randomly and equally assigned to receive radiotherapy alone or radiotherapy plus PCV chemotherapy (with drugs procarbazine, lomustine and vincristine). Before and after around half of the patients had been followed for over 11 years, genetic analyses were performed.
The median overall survival time was similar for patients receiving radiotherapy alone or radiotherapy plus PCV chemotherapy.
The good news comes when it is about the patients with the rare form of brain tumor, 1p19q co-deleted tumors.
The 126 patients with co-deletion lived more (a median survival rate of 8.7 years) than the 135 patients with tumors without the co-deletion (2.7 years).
The 59 patients with co-deletion tumors who received PCV chemotherapy plus radiotherapy lived much longer, double time (14.7 years) than the 67 patients with co-deletion who received radiotherapy alone (median survival rate 7.3 years).
Where the tumors did not have the chromosomal abnormality, no improvement in survival from the addition of chemotherapy was found.
“The Radiation Therapy Oncology Group and other participating cooperative groups are to be congratulated for conducting this randomized clinical trial in a rare form of brain tumor that took many years. Their persistence and dedication was rewarded as this genetic abnormality has a powerful effect on survival, and the results will change how patients with this disease are treated. This clinical trial also highlights the necessity for collecting tumor tissue for genetic studies to define more precisely the patients who benefit most from specific therapies,” said Jeffrey Abrams, M.D., associate director, Cancer Therapy Evaluation Program, NCI.
“That’s remarkable when most new cancer therapies offer only a few more weeks or months of survival,” said Dr. Bhupinder Mann, National Cancer Institute scientist.
“It’s very gratifying and good news for the patients diagnosed with these types of tumors. But they are, unfortunately a minority,” said Dr. Steven Rosenfeld head of the brain tumor center at the Cleveland Clinic.
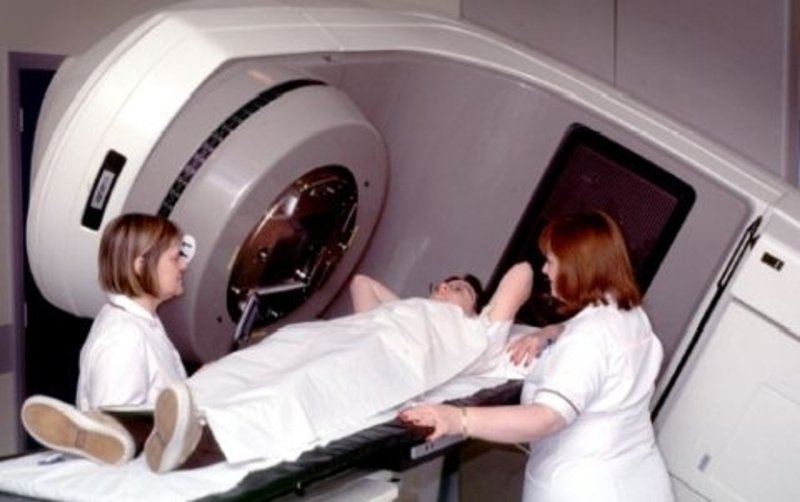
Radiation therapy alone has been the most common treatment used in brain tumor. Now the personalized medicine shows a benefit from adding chemotherapy in certain type of brain cancer.
The average age at diagnosis for this type of brain tumor, anaplastic oligodendroglioma, is 35.
These tumors represents 9.4% of all primary brain and central nervous system tumors.
Around 1,000 Americans a year develop oligodendrogliomas and co-deletion is found in around half of the cases.
Radiotherapy alone has been the common treatment used for oligodendrogliomas.
“This tumor hits people in their 30s and 40s, in the prime of life. It really highlights the importance of personalized medicine. We know these tumors are not all the same,” said Dr. David Reardon, clinical director of neuro-oncology at Boston’s Dana-Farber Cancer Institute.
Although this combination of therapies does not cure brain cancer, it gives a hope to young persons with certain brain tumor.
